HPV immunization policies
- Downloads
- Full report (pdf)
- Webinar slides (pptx)
Background and key statistics on HPV immunization in Canada
![]() In 2020, it is estimated that 1,350 Canadian women will be diagnosed with cervical cancer, and 410 will die from the disease.
In 2020, it is estimated that 1,350 Canadian women will be diagnosed with cervical cancer, and 410 will die from the disease.
Compounding this tragedy is the reality that cervical cancer is almost entirely preventable and, if detected and treated early, highly curable. While there are over 100 types of HPV, some strains have a higher risk of causing cells to become abnormal and precancerous.
Risk factors for HPV
- number of lifetime sex partners
- previously sexually transmitted infection
- history of sexual abuse
- early age of first sexual intercourse
- tobacco or cannabis use
- immune suppression
- inconsistent condom use
- men who have sex with men (MSM are 20 times more likely than heterosexual men to develop anal cancer)
Impact of HPV immunization on cervical cancer
- Since the introduction of population-based cervical screening, cervical cancer incidence has consistently declined in Canada. For information about HPV primary screening and abnormal result follow-up, see the Cervical cancer screening in Canada: Environmental scan (2019-2020) from the Partnership
- HPV immunization is associated with a substantially reduced risk of invasive cervical cancer at the population level.1
- HPV immunization before 17 years old: 90% reduction in invasive cervical cancer risk
- HPV immunization before 30 years old: 50% reduction in cervical cancer risk
Age-standardized incidence rates (ASIR) cervical cancer, females, Canada*, 1984-2019
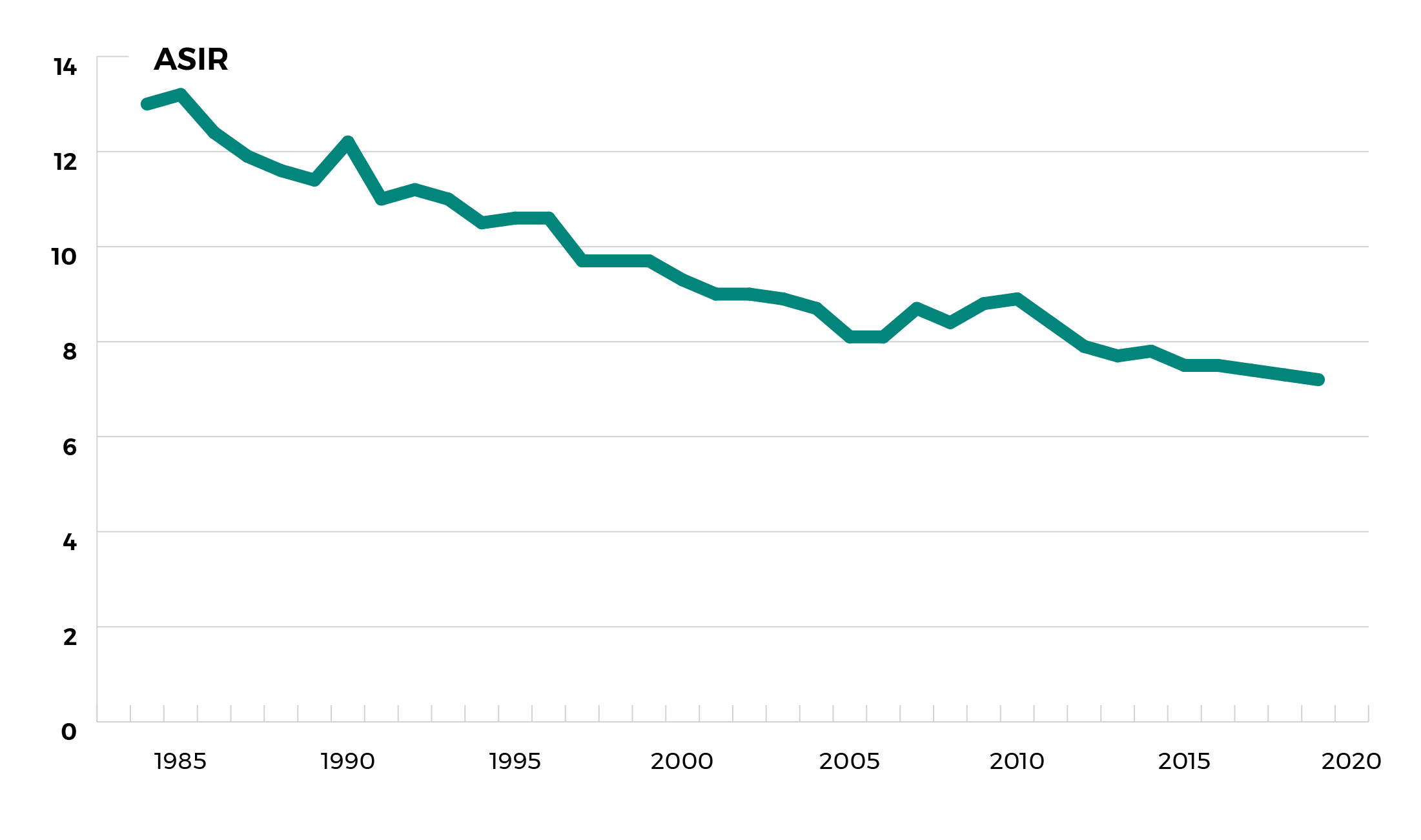
*Excludes Quebec
HPV immunization uptake
- All provinces and territories have a school-based HPV immunization program for girls and boys.
- HPV vaccination is offered on a 2 or 3 dose schedule.
- Immunization uptake data is available for different school years across jurisdictions. The provincial/territorial immunization uptake (for final dose) based on the most recent data ranges from 57.1 to 91.3% for girls and 57.5 to 91.3% for boys.
Provincial and territorial final dose uptake rates for HPV immunization for girls
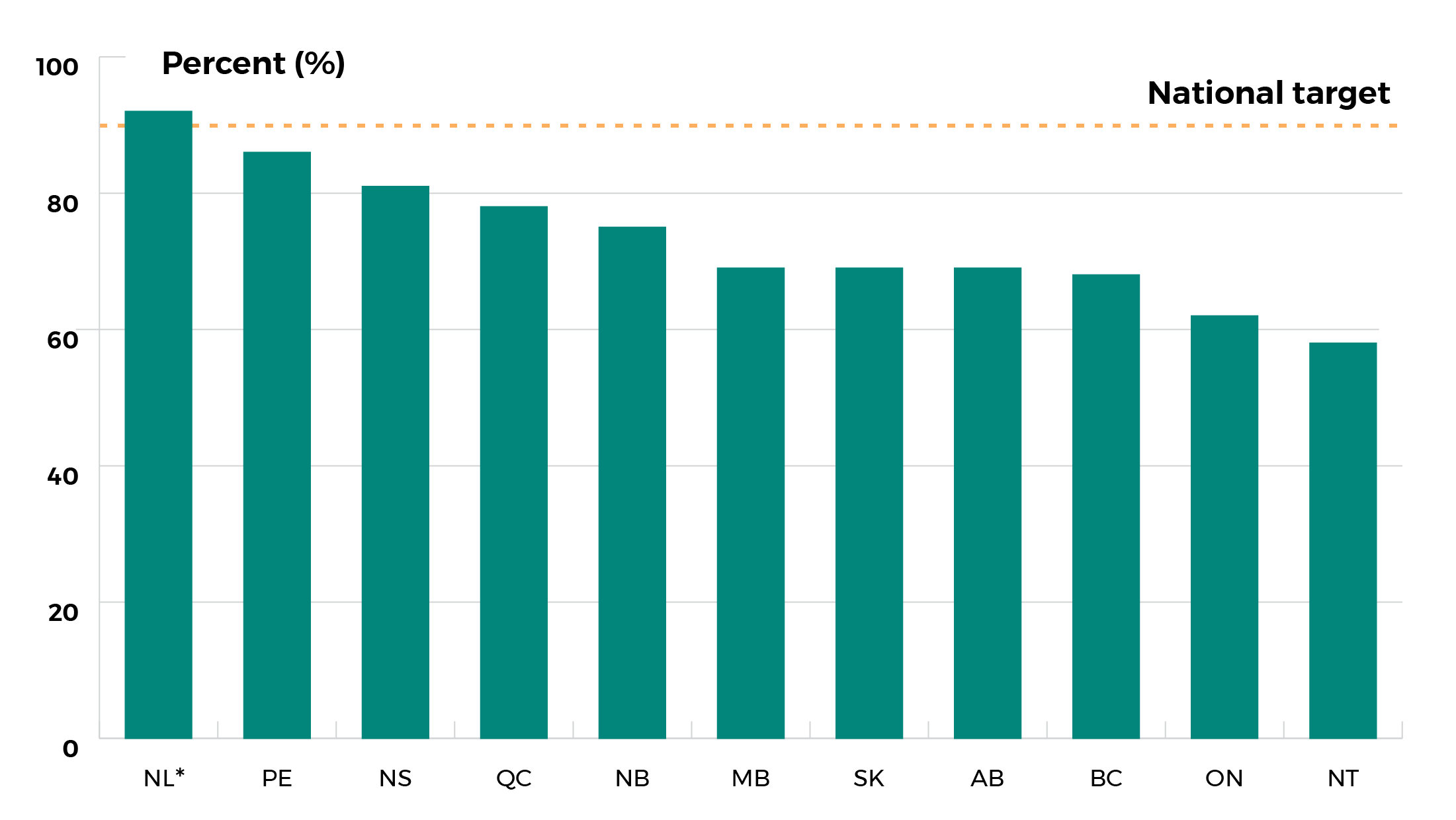
*rate for girls and boys combined
Provincial and territorial final dose uptake rates for HPV immunization for boys
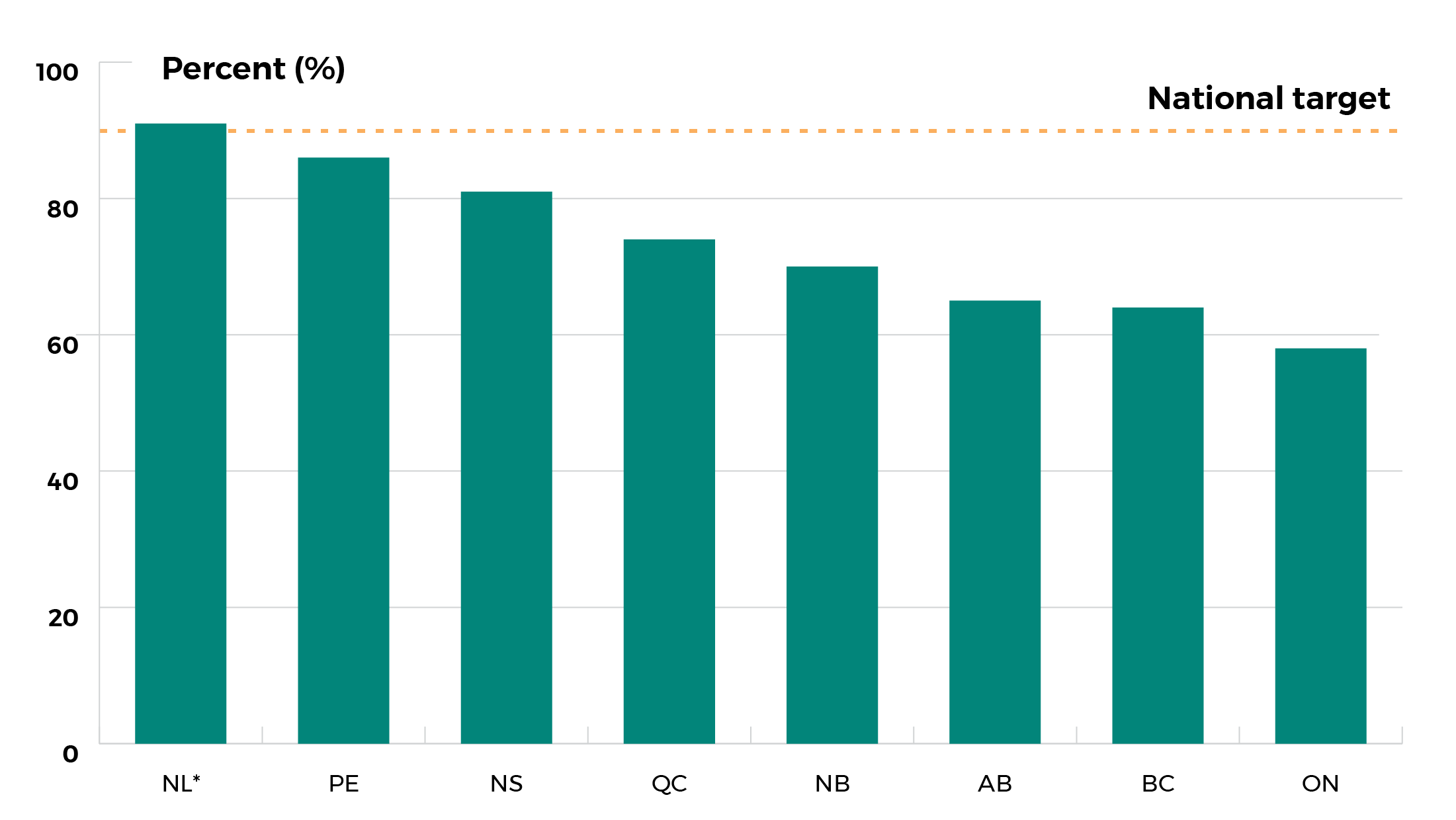
*rate for boys and girls combined
HPV vaccines licensed in Canada
| Vaccine | Target | Authorized use in Canada |
|---|---|---|
| Bivalent vaccine2 (Cervarix) | HPV types 16, 18 | Females 9-45 years of age |
| Quadrivalent HPV vaccine3 (Gardasil) | HPV types 6, 11, 16, 18 | Females 9-45 years of age Males 9-26 years of age |
| Nonavalent vaccine4 (Gardasil 9) | HPV types 6, 11, 16, 18 31, 33, 45, 52, 58 | Females 9-45 years of age Males 9-45 years of age |
Since 2017, HPV vaccination has been available in publicly funded school-based immunization programs in all provinces and territories and are administered starting as early as grade 4, but more commonly in grades 6 or 7. HPV vaccination is recommended by the National Advisory Committee on Immunization (NACI) for all individuals between ages 9 and 26.
International context
- Cervical cancer is the third leading cancer among women globally, and is estimated to cause the death of over 300,000 women annually.5
- It is the second most common cancer in women between the ages of 15-44.6
- The vast majority of cases globally (85%) occur in less developed countries, where cervical cancer represents 12% of all female cancers.
- Given that cervical cancer is almost entirely preventable, in 2018, the World Health Organization (WHO) called upon countries around the world to eliminate cervical cancer by the end of the century, identifying a target of less than 4 instances of cervical cancer per 100,000.
Age-standardized incidence rate of cervical cancer by country7 (estimates for 2018)
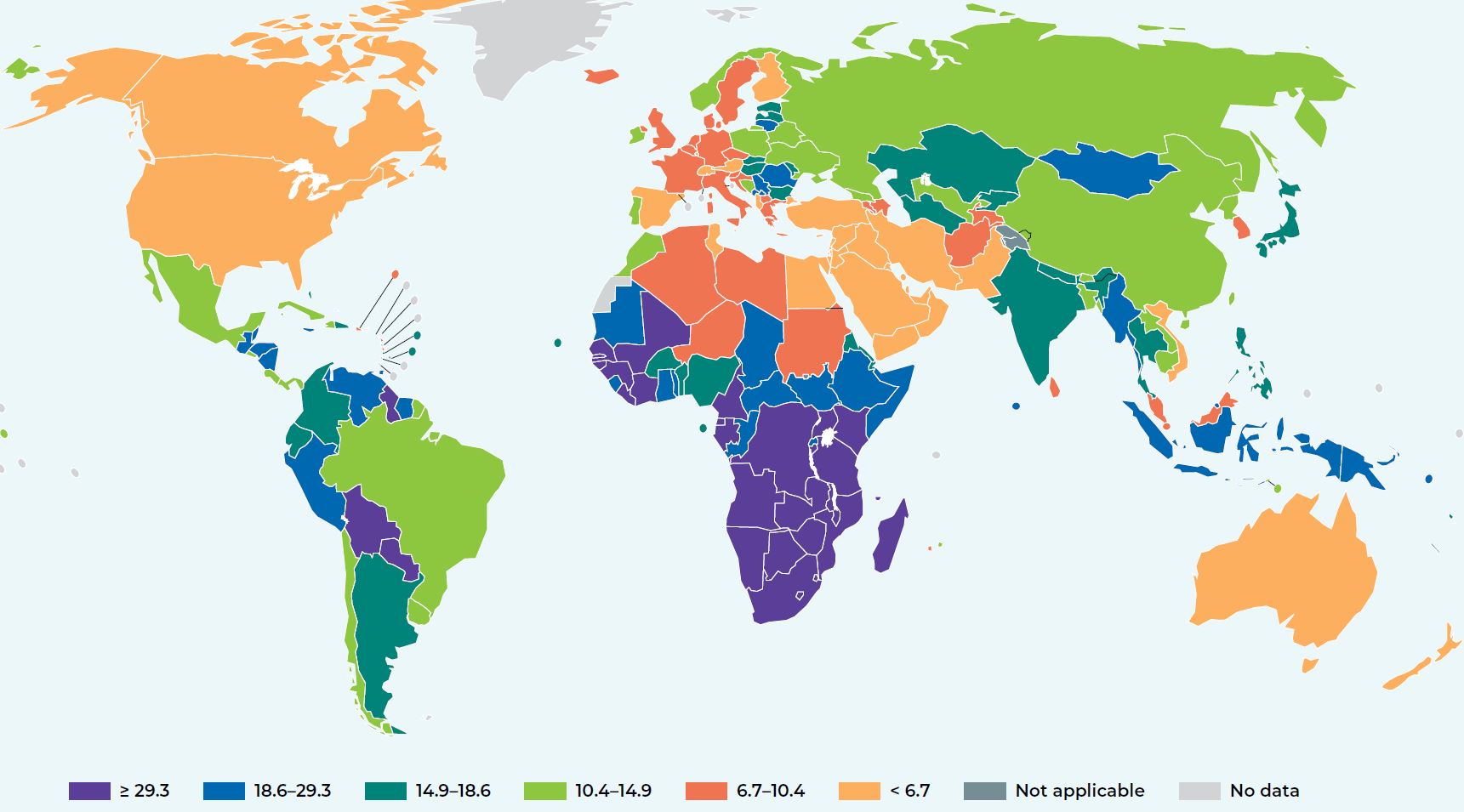
-
References
1 - Lei J, Ploner A, Elfström KM, Wang J, Roth A, Fang F, Sundström K, Dillner J, Sparén P. HPV Vaccination and the Risk of Invasive Cervical Cancer. New England Journal of Medicine. 2020 Oct 1;383(14):1340-8.
2 - Cervarix Canadian Product Monograph, GlaxoSmithKline Inc.; November 25, 2014
3 - Gardasil Canadian Product Monograph, Merck Canada Inc.; March 10, 2015
4 - Gardasil 9 Canadian Product Monograph, Merck Canada Inc.; Aug 30, 2020
5 - Prevention and control of cervical cancer. World Health Organization. 2020. Cited 22 October 2020. Available from: https://www.who.int/reproductivehealth/topics/cancers/en/
6 - Human Papillomavirus and Related Diseases Report. HPV Information Centre. 2020. cited 22 October 2020. Available from: https://www.hpvcentre.net/statistics/reports/XWX.pdf
7 - IARC. Cervix uteri. Gco.iarc.fr. 2018 cited 24 October 2020. Available from: https://gco.iarc.fr/today/data/factsheets/cancers/23-Cervix-uteri-fact-sheet.pdf
- Downloads
- Full report (pdf)
- Webinar slides (pptx)
